Real-world impact of physical activity reward-driven digital app use on cardiometabolic and cardiovascular disease incidence
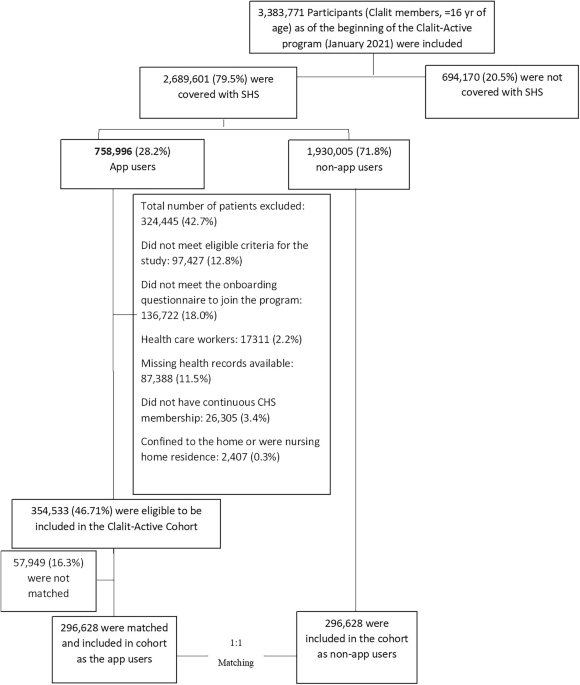
Population and study design
We performed a retrospective cohort study using the datasets of Clalit Health Services (CHS), the largest integrated healthcare service provider and payer system in Israel. CHS offers primary, speciality, and inpatient care to over 51% of the Israeli population, boasting 4.9 million members. CHS comprehensive healthcare data warehouse integrates hospital and community medical records and encompasses administrative and clinical data, laboratory and imaging information, pharmaceutical records, socio-demographic details, diagnoses from both community and hospital settings and biomarkers. Membership turnover within CHS is less than 1% annually, facilitating the study of population trends over time16.
The electronic health records (EHRs) used in this study are derived from Clalit Health Services, which has established rigorous validation protocols to ensure data reliability. Previous validation studies have confirmed the accuracy and comprehensiveness of Clalit’s EHR data17,18.
Eligible participants were CHS members at age ≥25 years old, with at least one year of continuous CHS membership that own CHS supplemental health services (SHS) who registered to use the app between January 2021 and June 2023. We excluded members who didn’t complete the onboarding questionnaire, CHS healthcare workers, missing health information, members without one year of CHS membership or those marked as bed-ridden.
App users were those who downloaded the app, completed the baseline questionnaire and had signed into the app at least three times within the first 30 days (i.e., app activation) emphasizing meaningful engagement during the initial month of app use. All other eligible members were marked as non-users (See Supplemental Fig. 1).
The app users were then matched 1:1 with non-app users (i.e., CHS members that meet the same baseline eligibility criteria as those listed above but did not download and activate the app). The follow-up period for both app and non-app users was defined as the initial registration date of the matched app user (i.e., index date).
The matching was performed based on socio-demographic and clinical covariates. The socio-demographic variables included gender, age at index date, place of residency (urban or rural area) and religious sector (Jewish, Arab, and Ultra-Orthodox), Gender was assigned based on electronic health records (EHR) as documented in the Clalit Health Services database, clinical variables included pre-existing chronic conditions (cancer, heart disease, sickle cell disease, asthma, stroke, hypertension, neurological disease, liver disease, thalassemia, respiratory disease, prior diagnosis of type 2 diabetes, prior diagnosis of CVD, solid organ transplant recipient or immunodeficiency), BMI category (underweight, normal weight, overweight, obese, and morbidly obese), and most recent HbA1C laboratory test value. Definitions for these variables and category thresholds are available in Supplemental Table 1.
Exact matching was performed for dichotomous and categorical variables, while the 1-nearest neighbor algorithm was employed for continuous variables to identify the closest match. App users who did not have an exact match were excluded from the analyses. We assessed covariate balance between app users and non-app users both before and after 1:1 matching (see Supplemental Fig. 2 for further details).
The intervention
The app is cellphone-based, and it was established by CHS leadership to prompt a healthy lifestyle among its members. The app is free to use for all CHS members who have supplementary health services (SHS). About 80% of CHS members are enrolled in the SHS plan. The app was initially introduced to CHS members through Clalit-funded media campaigns that were launched in January 2021. Users are prompted to enhance their engagement in physical activity by setting personalized weekly health-related goals based on their individual characteristics and previous physical activity (PA) history. An ongoing incentive system, rooted in behavioral science, offers personalized rewards aimed to increase adherence. The Clalit-Active app collects a broad range of information and since this app is embedded within Clalit, individual-level anonymized data is extracted from the app registry and its data is integrated into Clalit electronic health records (EHR) on daily basis, allowing the opportunity to assess the impact of Clalit-Active on health outcomes (for detailed information of the app features see Supplemental Table 1). Participant data was retrospectively linked with Clalit Electronic Health Records (EHR) at the time of app use, transferred and integrated with a daily granularity. This interoperability between app logs and health records facilitates the longitudinal integration of medical information, continually updated physical activity and lifestyle-related data for all Clalit-Active users. Notably, approximately 30% of app users engage with the platform on a daily basis.
Study participant classification
The study participants were categorized as follows: App users were individuals who downloaded the app, completed the baseline questionnaire, and logged into the app at least three times within the initial 30 days, indicating substantial engagement during the early phase of app utilization. Non-app users were identified as CHS members who did not download or activate the app. Among the app users, levels of physical activity were categorized based on the number of daily steps recorded during the first 30 days. The levels were consistent with the US physical activity guidelines and were defined as: mild (up to 5000 steps per day), moderate (5000-9999 steps per day), and high (10,000 steps per day or more)19. While these thresholds align with step-based categories commonly used in research, they are not directly derived from the US Physical Activity Guidelines, which do not specify step-based goals. Instead, these categories were chosen to approximate mild, moderate, and high levels of activity based on general guidelines and previous studies that correlate step counts with physical activity intensity8,20.
Outcomes
For the current study, we included three main outcomes: (1) new-onset (first) of cardiovascular disease (CVD), (2) new-onset (first) of type 2 diabetes and (3) first stroke. Additionally, we created a fourth composite outcome, encompassing any of these three diagnoses. All extracted at an individual level from the patient’s Electronic Health Records. For all four outcomes, only newly diagnosis conditions reported and documented after the index date and through the follow-up period were considered (refer to Supplemental data 1 for detailed definitions of variables). In cases where users had a past or prevalent diagnosis of the three outcomes as of the index date, these individuals were excluded from the corresponding outcome-specific analysis.
We followed all eligible members and their matched controls until the end of the study period (September 30th, 2023), outcome of interest, death, or loss to follow-up, whichever occurred first. For app users, loss of follow-up was defined as the date when they stopped using the app for at least three months.
Covariates
Adjusting for confounders of the association between physical activity, and subsequent health outcomes was performed through the matching and the cox proportional hazards regression model. Certain adjustment variables were shared across all outcome models, while others were specific to certain models only. Common confounders included BMI at baseline, number of GP visits ever recorded before the index date, and prior diagnosis of the following conditions: hypertension, type 2 diabetes, CVD, hyperlipidemia, and cancer.
All variables were extracted according to the most recently documented value reported in the EHR before the index date. Full variable definitions are presented in Supplemental Table 1.
Statistics and reproducibility
Following the matching, descriptive statistics were performed to compare the sociodemographic and clinical characteristics of app users to non-app users. We summarized the distribution of categorical variables per group and provided the average and standard deviation or median and IQR for continuous variables based on their distribution. Additionally, we characterize the levels of physical activity (mild, moderate, and high) by the type of incentives. The cumulative incidence for each outcome of interest was calculated using the Aalen-Johansen estimator21. Cox models were conducted to determine the outcome-specific hazard ratios (HR) of incidence of the three study outcomes as well as the composite outcome. We performed four different Cox proportional hazards regression models that were each adjusted for a predefined distinct set of covariates based on scientific literature and clinical judgment. All models were adjusted for the following confounders: age, gender, socioeconomic status, number of physician visits up to the index date. The models for incident CVD and stroke included the following variables at adjustment: history of hypertension, type 2 diabetes, hyperlipidemia, and latest BMI recorded prior to the index date. The model for incident type 2 diabetes included: history of hypertension, CVD, hyperlipidemia, and latest BMI recorded prior to the index date. The model for the composite outcome included: age, gender, socioeconomic status, history of hypertension, hyperlipidemia, latest BMI recorded prior to the index date and number of physician visits up to the index date. These analyses were exploratory in nature and allowed a data-driven approach to identify the incident diseases having a statistically significant association with physical activity while adjusting for relevant covariates. Additionally, a similar analysis was performed by the three levels of physical activity compared to non-app users. Based on pre-existing literature regarding the differences in physical activity levels between genders, a subgroup analysis was conducted by the levels of physical activity and gender for all the study outcomes. The proportional hazards assumption was examined using the cox.zph function22 of the survival R package and was met for all models.
Sensitivity analysis
To assess the robustness of our results about the effect of app usage on health outcomes, a sensitivity analysis was performed using a different matching approach. We employed a Propensity Score Matching (PSM). Each app user was matched with a non-user, based on the similarity of their propensity scores (1:1 matching ratio). Multivariable logistic regression was conducted to generate propensity scores.
Ethics
The study was approved by the CHS Institutional Review Board (IRB) (0068-21-COM1(. As this was a retrospective study using de-identified patient data, the requirement for informed consent was waived. However, all individuals who signed up for the Clalit-Active app provided informed consent for data collection as outlined in the app’s terms of use. The CHS database was initially established and approved for research use by the CHS IRB, which continues to oversee data governance, privacy protections, and research activities involving the dataset. All analyses in this study were conducted in accordance with institutional and ethical guidelines.
Reporting summary
Further information on research design is available in the Nature Portfolio Reporting Summary linked to this article.
link



:max_bytes(150000):strip_icc()/A-Physical-Therapist-Shares-the-Most-Underrated-Physical-Activity-94666d193c98412ca90ffbcc23339f90.jpg)



