Influence of the SARS-CoV-2 pandemic and infection on musculoskeletal function
This prospective study aimed to explore the impact of the global SARS-CoV-2 pandemic on indicators of musculoskeletal health. The SARS-CoV-2 pandemic was approached from multiple angles, using data obtained from both SARS-CoV-2 non-infected and SARS-CoV-2 infected individuals. With this approach, the study first aimed to examine how the pandemic and the resulting changes in daily life could affect the musculoskeletal system. Secondly, it aimed to investigate the potential effects of a SARS-CoV-2 infection on established indicators of musculoskeletal health. The data of this trial show no association between SARS-CoV-2 infection and musculoskeletal changes in the cohort studied, overall indicating that SARS-CoV-2 infections may not be a significantly associated with major deterioration of musculoskeletal function. The findings further suggest that lifestyle changes in daily routines and physical activities associated during the pandemic might negatively affect specific parameters of musculoskeletal health.
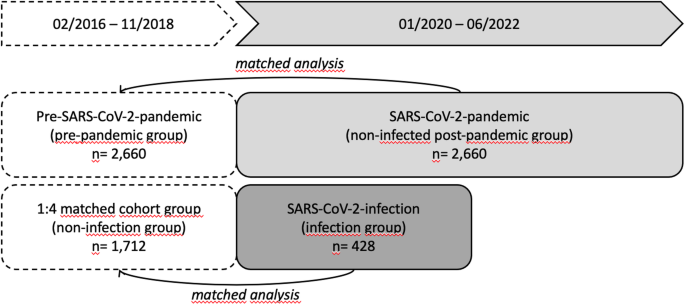
To assess the influence of the SARS-CoV-2 pandemic on the musculoskeletal system, two cohorts of non-infected participants were compared: one before the pandemic and one during the pandemic at one single time point. In this context, the baseline characteristics of the participants, including sociodemographic information, comorbidities, and anthropometric data, were comparable and similar in both groups. This suggests that the groups were adequately matched. The study revealed that the average skeletal muscle mass, a measure of muscle quantity, was significantly lower in the post-pandemic group as compared to the pre-pandemic group. The observed decrease in skeletal muscle mass within the post-pandemic group might be attributed to a combination of factors influenced by the pandemic-induced lifestyle changes. Lockdowns, social distancing measures, and increased time spent indoors could have contributed to a reduction in physical activity19,20,21. This hypothesis is supported by the fact that participants in the post-pandemic group reported a statistically significant lower average number of hours of physical activity per week. Reduced physical activity has been associated with muscle atrophy22,23 and a shift in body composition towards a higher fat content24. Additionally, other factors, such as changes in dietary habits, might have played a role25,26. Tzeng et al. examined lifestyle behaviors in older adults independently of the SARS-CoV-2 pandemic to assess their risk of musculoskeletal impairment. They demonstrated that an unbalanced diet and reduced physical activity were associated with an increased risk of functional and structural muscle loss in this age group27. Batista et al. and Saraiva et al. specifically examined the impact of the SARS-CoV-2 on the mobility of older adults and the associated risk of musculoskeletal impairment. Their findings indicated an increased prevalence of impairments in muscle mass and function in this group. In particular, reduced life space mobility was a significant contributor to muscle loss in older adults during the SARS-CoV-2 pandemic28,29. Similarly, the psychological aspects associated with the pandemic could have contributed. Stress-induced changes in hormone levels may influence alterations in body composition. Moreover, heightened stress levels can potentially lead to the adoption of unhealthy eating patterns and consequent weight gain30,31. Other research has shown similar results: Hasegawa et al. investigated the impact of SARS-CoV-2 pandemic measures on muscle mass in older type 2 diabetes patients. Their analysis of bioelectrical impedance data from 56 patients, with an average age of 75.2 years, revealed a significant decline in muscle mass during the SARS-CoV-2 pandemic. They propose that the restrictions on physical activity may have contributed to the muscle loss in these older patients32. Kirwan et al. conducted a comprehensive review of the causes of muscle mass loss and compared them with data showing how the SARS-CoV-2 lockdowns affected physical activity, diet, sleep and stress. Their findings suggest that the lockdowns, which lowered physical activity levels and altered dietary habits, may increase the risk of muscle loss, especially in older individuals7. In a similar study, Woods et al. discussed the further effects of the SARS-CoV-2 pandemic on health and daily life. The study indicates that the reduced physical activity caused by quarantine and social distancing may have a negative impact on our muscles and general physical health33.
However, it is important to acknowledge that impairments in mobility and musculoskeletal function in this study may not entirely capture the effects of social isolation on functional abilities. Although a reduction in skeletal muscle mass was observed, the evaluation of muscle strength via handgrip and physical performance assessed through the timed up and go test showed no significant differences between the groups. The absence of substantial differences in these metrics suggests a relatively restrained effect of the pandemic on these particular parameters in this particular study cohort at a single time measurement. However, in the post-pandemic cohort, the average age with a median age is 54.0 years in both groups. Since reduced musculoskeletal function is a syndrome associated with aging34, it might be plausible that the observed effects primarily represent precursors, potentially indicative of a higher propensity for the development of progressive muscle mass and function loss in individuals over time. Caution is needed when interpreting this hypothesis, but it could provide useful insights for future research, particularly in studies targeting the pandemic effects especially on older populations.
In order to evaluate the impact of a SARS-CoV-2 infection on the musculoskeletal system, study participants who had experienced a SARS-CoV-2 infection were matched with a non-infected cohort. While the baseline characteristics were effectively matched, differences in physical attributes such as BMI, height, and weight surfaced between the infection and pandemic cohorts were found. Participants in the infection group had significant differences in height and weight, being significantly taller with a median of 2.60 cm and heavier with a median of 2.45 kg. However, physical activity levels were similar in both groups, with participants from each group reporting engagement in regular physical exercise. Furthermore, the average weekly duration spent on physical activities demonstrated consistency across the two groups. The similarity in activity engagement suggests that participants in both cohorts likely maintained comparable levels of physical activity. This, in turn, might have played a role in preserving musculoskeletal health, even in the context of acute infections and subsequent periods. Despite the initial finding of reduced skeletal muscle mass in the non-infected group, when accounting for body surface area through regression analysis, the differences in skeletal muscle mass, hand grip strength, and timed up and go test between the infection and non-infection groups were not statistically significant. This suggests that the initial observed differences may have been influenced by variations in body size and are not in association with a SARS-CoV-2 infection. Similar findings were reported by Liu et al. They investigated the association between a SARS-CoV-2 infection and reduced muscle function and mass using data from the UK Biobank. To identify potential associations, they performed various Mendelian randomization analyses to test for causality. However, their results did not provide strong evidence of a direct causal relationship between a SARS-CoV-2 infection and reduced muscle function and mass. While the study investigated the direct causal relationship between a SARS-CoV-2 infection and the loss of muscle mass and function, the results suggest a possible indirect interaction35. However, other studies analyzing the effect of a SARS-CoV-2 infection have shown that particularly severe cases of an infection, characterized by prolonged disease, can lead to muscle atrophy and dysfunction36,37. Notably, our study did not include this specific group of patients with severe disease progression.
In terms of progressive and generalized loss of muscle mass and function, the current data show that the prevalence was relatively low in both the infection and non-infection groups. This study contributes to the understanding of the relationship between a SARS-CoV-2 infection and the musculoskeletal system by highlighting that, in the context of mild to moderate infections and short durations, the virus does not appear to lead to substantial musculoskeletal deterioration or a significantly increased risk of progressive and generalized loss of muscle mass and function. However, it’s important to note that the study’s findings are based on specific parameters and characteristics of the participants, and that the impact of SARS-CoV-2 infection on musculoskeletal health may still vary depending on factors such as disease severity, duration, and individual health conditions. Furthermore, it is important to note that the generalizability of these findings is limited by the relatively young and healthy nature of our study cohort, which may not reflect more vulnerable populations at higher risk or severe COVID-19 outcomes.
Limitations
There are several limitations to this study. First, the average age of the participants, ranging from early to mid-50 s, is comparably young in the context of progressive and generalized loss of muscle mass and function, which primarily effects older patients. This demographic characteristic is also reflected in the relatively low prevalence of sarcopenia observed in this study. To address this limitation, future studies should specifically focus on elderly populations to investigate the impact of SARS-CoV-2 infection, pandemic-related lifestyle changes, and similar public health crises on musculoskeletal health. Another important limitation is the potential for selection bias, as the study cohort predominantly consisted of relatively healthy and mobile individuals. The demanding nature of the 7-h study visit likely discouraged participation by those with significant health impairments or physical limitations. Consequently, the resulting cohort may not adequately represent more vulnerable or clinically relevant populations38. In addition, the available data only include assessments of participants with asymptomatic to mild infection. The dataset lacks information on more severe infection courses and their impact on musculoskeletal health. Furthermore, there is no data available on virus variants or vaccination status of the post-pandemic cohorts. Finally, the use of BIA to assess muscle mass can be considered a limitation, as this method has certain constraints compared to gold-standard techniques such as DXA39. However, BIA is recommended by current guidelines for the assessment of body composition and muscle-related conditions, including sarcopenia, given that all participants were measured under standardized conditions, the results remain internally comparable and valid for group comparisons.
link



:max_bytes(150000):strip_icc()/A-Physical-Therapist-Shares-the-Most-Underrated-Physical-Activity-94666d193c98412ca90ffbcc23339f90.jpg)



