Buddhist ordination as a culturally embedded model for improving diet, body composition, and sleep quality in overweight and obese adults
Study design
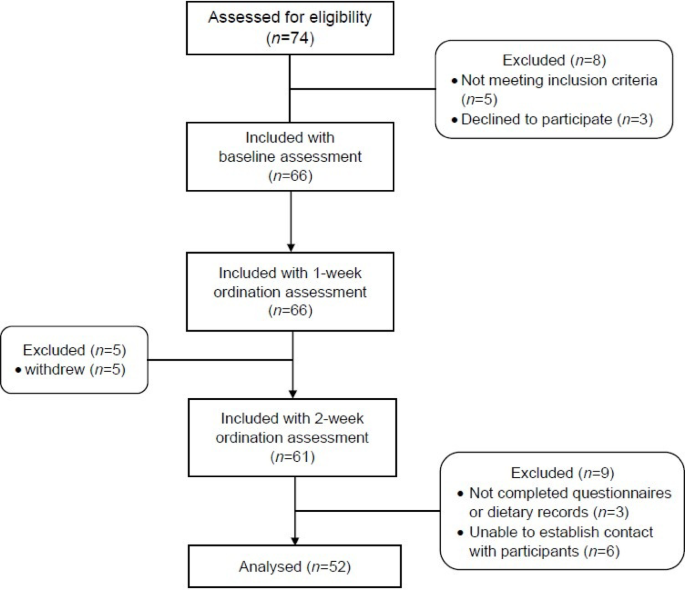
A prospective observational study was conducted between January and May 2024 at Wat Bowaniwet Wihan Ratchaworawihan, a Dhammayut Buddhist temple in Bangkok, Thailand. The study was designed to capture physiological changes during the early phase of ordination, a period characterized by substantial lifestyle transitions. Participants were assessed at three key time points: baseline (first day of ordination), after one week, and after two weeks (final week of ordination). At baseline, participants maintained their regular lifestyles, including their typical diet, sleep schedule, and physical activity patterns until ordination. During ordination, participants adopted monastic routines as dictated by Buddhist disciplinary codes, including pre-noon food consumption, increased sedentary activity (meditation and chanting), and structured sleep-wake schedules.
The duration of the study was set at two weeks, aligning with the minimum period of monastic ordination commonly practiced in Thai Buddhism. According to temple tradition, newly ordained monks must remain in the monastic order for at least two weeks before disrobing (“suek”). This provided a natural and culturally defined timeframe for data collection, ensuring that all participants were observed under consistent monastic conditions from ordination to the point of potential disrobing.
Importantly, participants were permitted to consume unrestricted quantities and types of food and beverages offered through alms during the eating window, reflecting real-world monastic practice. Researchers did not interfere with dietary choices to preserve ecological validity but provided telephone access for any study-related questions. The design aimed to evaluate how these organically structured routines affect dietary patterns, anthropometry, and sleep in a short timeframe.
In addition, the study protocol received approval from the Ethics Review Committee for Research Involving Human Research Subjects, Human Science Group, Chulalongkorn University (COA No. 013/67), adhering to the Declaration of Helsinki guidelines. Before enrollment, all participants provided written informed consent, and their information was maintained with strict confidentiality.
Sample size calculation
The sample size was determined based on the 0.05 level of significance (α), 80% power, effect size (0.44), using the BMI of obese men that enrolled in TRE protocol from the previous study50. Using this as the total population and considering an estimated drop-out rate of 30%, a target sample of at least 56 participants was set to ensure adequate statistical power to detect meaningful changes in dietary intake, body composition, and sleep parameters over time. A total of 52 participants completed the full study protocol.
Participants details
Fifty-two newly ordained Dhammayut Buddhist monks were recruited from Wat Bowaniwet Wihan Ratchaworawihan, Bangkok. Inclusion criteria were adults aged 20 years or older, with a BMI greater than 22.9 kg/m²51, willingness to undergo ordination for at least two weeks, fluency in Thai, and agreement to participate in the study. Exclusion criteria included early withdrawal from monkhood before the two-week period or incomplete data on questionnaires, dietary records, or body composition measurements.
Outcomes measurement
The primary outcome of the study was body weight, as a sensitive and direct marker of short-term physiological change. Secondary outcomes included other components of body composition, dietary intake, and sleep quality parameters such as sleep timing, duration, onset latency, efficiency, disturbances, use of sleep medications, and daytime functioning.
Dietary intake
At baseline, participants received standardized training from registered dietitians on how to accurately record food and beverage consumption. The training utilized visual aids, food models, and standard household measuring tools (e.g., cups, spoons, and bowls) to enhance portion size estimation and recording accuracy. Each participant was provided with a structured food recording handbook and was instructed to complete a 3-day dietary record each week, covering two weekdays and one weekend day.
In addition, a 24-hour dietary recall interview was conducted at baseline to capture dietary intake prior to ordination. This recall was administered by registered dietitian to ensure accuracy and minimize recall bias. All dietary records and recall data were reviewed for completeness and consistency before analysis. Moreover, any potential underreporting or overreporting of data was verified by contacting the participants directly to ensure accuracy. Nutrient intake—including total energy, macronutrients, dietary fiber, and sugar—was analyzed using the INMUCAL-Nutrients software (version 4.0), developed by the Institute of Nutrition, Mahidol University, Thailand, which is based on a validated Thai food composition database.
Body composition
Assessments were conducted in the early morning, prior to breakfast, at two time points: baseline (the day of ordination) and after two weeks of monastic life. Participants wore light clothing and removed any metallic items or accessories to minimize measurement variability. Body composition parameters, including body weight, body mass index (BMI), body fat percentage, visceral fat level, and muscle mass, were measured using a validated bioelectrical impedance analysis (BIA) device (TANITA BC-401, Tokyo, Japan).
Waist and hip circumferences were measured using a non-elastic measuring tape. Waist circumference was recorded at the midpoint between the lowest palpable rib and the superior border of the iliac crest, while hip circumference was measured at the widest point of the buttocks. To ensure consistency and cultural appropriateness, all anthropometric measurements were performed by trained male researchers, adhering to Buddhist monastic discipline52. The same equipment, measurement time, and standardized protocols were applied across both time points to minimize inter-rater and device variability.
Sleep quality
Sleep quality was assessed using the Thai version of the Pittsburgh Sleep Quality Index (PSQI)53, a validated and widely used instrument for evaluating subjective sleep characteristics. The PSQI was administered at two time points: baseline (pre-ordination) and at the end of the second week of ordination. The instrument includes 19 self-rated questions grouped into seven component scores: subjective sleep quality, sleep latency, sleep duration, habitual sleep efficiency, sleep disturbances, use of sleeping medications, and daytime dysfunction. Each component is scored from 0 to 3, with higher scores indicating greater impairment. These scores are summed to yield a global PSQI score ranging from 0 to 21. A global score greater than 5 is indicative of poor sleep quality. Sleep onset latency, one of the key subcomponents, was also specifically evaluated, with scores interpreted as follows: 0 = no difficulty falling asleep, 1 = mild difficulty, 2 = moderate difficulty, 3 = severe difficulty. Participants completed the questionnaire independently, with support provided by the research team when needed to ensure accuracy and completeness. All responses were reviewed for consistency immediately after collection.
Statistical analysis
Data were presented as mean ± standard error of the mean (SEM), while categorical variables such as education level and underlying disease were expressed as counts and percentages. Normality of distribution for key variables was tested using the Kolmogorov–Smirnov test. Paired samples t-tests were used to assess changes between time points. Repeated measures ANOVA was used to examine the effects of treatment, time, and interaction terms. A P-value < 0.05 was considered statistically significant. Statistical analyses were performed using IBM SPSS Statistics (version 22.0; SPSS Inc., USA).
Strengths and limitations
This study is the first prospective investigation to assess short term physiological adaptations to Buddhist ordination, simultaneously evaluating changes in dietary intake, body composition, and sleep quality. The use of validated instruments, repeated measures, and a naturalistic monastic setting enhances both internal validity and real-world applicability. However, the limited observation period constrains the ability to generalize outcomes to longer term adaptations. Dietary intake was self-reported, which introduces the possibility of recall bias, although standardized protocols were used to mitigate this limitation. Waist circumference measurements were taken at non-standardized anatomical landmarks. In addition, physical activity was not assessed, and no biochemical or hormonal markers (e.g., glucose, cortisol) were collected, limiting the ability to interpret underlying metabolic changes.
The short duration of the study, coupled with the limited sensitivity of bioelectrical impedance analysis (BIA), may have restricted the detection of meaningful changes in visceral fat and muscle mass. Cultural context also imposes important constraints: monks rely on food offerings from laypeople during alms collection, thereby limiting their control over the nutritional quality and macronutrient composition of their diet. This structural dependence may contribute to the observed nutritional outcomes and should be taken into account when interpreting results and designing future interventions. Moreover, the study sample was limited to monks residing at Wat Bowonniwet Vihara, which may restrict the generalizability of the findings to other monastic communities. Future studies involving more diverse settings and longer follow-up periods are recommended to validate and expand upon these results.
link


:max_bytes(150000):strip_icc()/A-Cardiologist-Shares-the-Most-Meaningful-Change-You-Can-Make-for-Better-Heart-Health-e058d2d7f85a41ffa03cd0692f08e0de.jpg)




