Participatory development of an mHealth intervention delivered in general practice to increase physical activity and reduce sedentary behaviour of patients with prediabetes and type 2 diabetes (ENERGISED) | BMC Public Health

The mHealth intervention was developed according to the ‘mHealth development and evaluation framework’, which includes active participation of the target audience in focus groups and interviews [38,39,40]. This framework encompasses four sequential phases: (a) conceptualisation, (b) formative research, (c) pre-testing, and (d) piloting.
We present a combined overview of the methods and results for each phase, providing a cohesive narrative that aligns the development process with the corresponding outcomes, rather than separating out methods and results. We then present the finalised intervention, as implemented in the ongoing ENERGISED randomised controlled trial.
Participants
All participants involved in the intervention’s development were patients with (pre)diabetes who fulfilled the ENERGISED trial eligibility criteria (Additional file 1), recruited by collaborating GPs from their practices in Prague, Czech Republic.
The Ethics Committee of the General University Hospital in Prague (No. 49/20) provided study approval, and all participants provided informed consent.
Phase 1: conceptualisation
Methods
To reach a consensus on the key conceptual aspects of the intervention, the multidisciplinary team employed an informal decision-making process. This team comprised GPs (BS, MP, NK, TH), PA researchers (DVD, JP, MS, TY)– some of whom have extensive expertise with diabetes patients (TH, TY)– as well as psychologists and behavioural scientists (MU, SE, CW), and IT experts (JK, RC). The perspectives of GPs were deemed particularly crucial, as they are the primary agents tasked with the intervention implementation in real-world settings and they have day-to-day experience of consultations addressing physical inactivity with their (pre)diabetes patients. Engaging GPs early in the intervention development process was vital for identifying and overcoming potential barriers to implementation, such as time constraints and integration into existing workflows, while leveraging facilitators like the trusted GP-patient relationship and the GPs’ unique insights into patient needs and preferences [25, 31]. This approach aligns with prior research indicating that the early involvement of key stakeholders, especially those directly impacted by the intervention’s implementation, significantly enhances the feasibility and acceptability of health interventions [41]. The four GPs involved in the conceptualisation phase represented a diverse cross-section of practice settings, including both rural (MP) and urban (BS, NK) environments, and brought a range of experiences, with years of practice varying from recently qualified (MP) to over 30 years of experience (BS, TH). This diversity ensured a broad spectrum of insights into the challenges and opportunities of implementing the intervention across different healthcare contexts. The team included both male and female GPs, with three from the Czech Republic—where the intervention is to be implemented—to ensure the intervention’s relevance to the local healthcare system. Additionally, we included a GP from the UK (TH) with additional experience of delivering physical activity trials in primary care to incorporate an external perspective. This helped to enrich the intervention’s development, with broader insights into its potential applicability and scalability beyond the initial setting.The process began with individual team members thoroughly reviewing the latest evidence in their respective fields related to physical activity, diabetes management, behaviour change theories, mHealth technologies, and interventions related to all these areas, including our prior research [40, 42,43,44,45]. Following this, a series of meetings were convened, where team members presented their findings and proposed elements for the intervention’s design. During these meetings, facilitated discussions were held to integrate the diverse perspectives of the team, whilst considering resource and time constraints. The discussions were structured around several key conceptual aspects: underpinning theory and behaviour change techniques (BCTs); mode of physical activity and intervention goals; intervention components; and the required IT solution. The outcome of this process was a document, drafted by one of the researchers (TV), which outlined the agreed-upon key conceptual aspects forming the foundation of the intervention. This document, accompanied by a rationale for each aspect, was reviewed and approved by the entire team, guiding the subsequent phases of intervention development.
Results
Theoretical underpinning and behaviour change techniques
The mHealth intervention was underpinned by the theory of self-regulation, a psychological framework that emphasises the role of self-directed processes in guiding one’s behaviour towards achieving personal goals [46]. The intervention thus incorporates a range of self-regulatory BCTs, such as self-monitoring, goal setting, and feedback [47], to which we have allocated the same numerical codes in brackets as per Michie et al. taxonomy [48].
Self-monitoring (2.3) stands as a cornerstone of self-regulation, allowing patients to track their progress and gain insights into their PA patterns. A wealth of evidence indicates that self-monitoring can significantly increase PA levels [45, 49] and reduce sedentary behaviour [21, 43]. Goal setting (1.1) and regular goal review (1.5) further complement self-monitoring by providing patients with clear, tangible targets to strive for and a framework to evaluate their progress. Goal-setting is the key component of self-regulation [50] and one of the most potent behaviour change techniques in increasing PA [16, 51]. A recent meta-analysis estimated that setting a specific goal was associated with an increase of approximately 600 steps/day [42]. Action planning (1.4) and coping planning (1.2) aid in translating these goals into daily routines, helping patients identify specific activities, times, and contexts in which they can incorporate more PA. Action planning has been identified as one of the most frequently used BCTs in the general population [51] and patients with diabetes [52]. Furthermore, combining action planning, coping planning, and self-monitoring was more effective in increasing PA and reducing sedentary behaviour than using these BCTs alone [21]. Feedback on behaviour (2.2) serves as a continuous loop of reinforcement, allowing patients to understand where they are excelling and where there’s room for improvement. In a review of mHealth interventions to influence PA and sedentary behaviour, approximately half (46%) utilised feedback on behaviour [53], which is also commonly used in interventions targeting diabetes patients [52]. Providing information about health consequences (5.1) highlights the tangible health benefits of increased PA and the health risks of sedentary behaviour. This technique aims to enhance motivation and drive behavioural change, especially in patients with chronic conditions [54, 55], including (pre)diabetes [52]. Lastly, prompts and cues (7.1) play a crucial role in nudging patients towards increased PA and reduced sedentary behaviour in real-time. While not commonly used in traditional PA interventions, prompts are massively utilised by mHealth interventions, which facilitate easy implementation of timely reminders or suggestions, often based on real-time wearable sensor data [53, 55, 56].
Collectively, these BCTs form the backbone of our intervention, each contributing uniquely to fostering a sustained increase in PA and a decrease in sedentary behaviour among our target population.
Mode of physical activity and intervention goals
We identified walking as the primary mode of PA for the intervention due to its accessibility, low cost, established benefits for metabolic health [57, 58], and safety [59]. This choice is grounded in the understanding that walking can be seamlessly integrated into daily routines, making it a sustainable option for most individuals [60], including patients with (pre)diabetes [57, 61]. Besides, walking can be easily quantified as a daily step count and self-monitored using pedometers or activity trackers.
Goal setting is pivotal to the intervention; thus, we developed a set of recommended patient goals including: (a) increasing daily step count; (b) enhancing walking cadence; and (c) interrupting prolonged bouts of sitting.
The consensus was to advise patients to boost their daily step count by at least 3,000 above their baseline, a common goal in behavioural interventions [59, 62, 63]. This increment equates to approximately 30 min of walking, assuming a pace of 100 steps per minute—a heuristic estimate for a moderate-intensity threshold [64]. This represents more than 150 min of moderate-intensity PA each week, in line with the WHO’s guidelines for adults with chronic conditions [65]. Recognising the significance of patient autonomy, if patients find the 3,000-step increase challenging, they can propose a more feasible goal, ensuring that the goal feels personally meaningful rather than externally imposed [66]. To offer added flexibility in planning, the daily step target will be translated into a weekly goal by multiplying by seven, in line with WHO guidelines providing weekly rather than daily goals [65].
To ensure that patients achieve at least moderate-intensity levels, they will be recommended to aim for a cadence of at least 100 steps per minute [64], initially in short durations, and gradually extending these periods to make this cadence habitual. For example, patients can monitor their step count for 5 min, trying to achieve at least 500 steps, ultimately aiming for 3,000 steps in 30 min [63, 67, 68]. However, if the 100 steps per minute benchmark proves challenging, they can elevate their cadence as much as comfortably possible [65].
Lastly, given the positive effect of interrupting prolonged sitting bouts on metabolic markers in (pre)diabetes patients [8,9,10], they will be urged to break up sitting every 30 min for at least 3 min, during which they should either walk, preferably at moderate intensities, or perform simple exercises, such as chair squats, calf raises, or walking in place.
Intervention components
The mHealth intervention consists of text messages implementing various BCTs, some triggered ‘just in time’ based on Fitbit activity tracker data. To tailor the mHealth intervention to individual patients and to facilitate its adoption, patients will be initially supported with regular phone counselling. GPs initiate the mHealth intervention during routine health check-ups and provide patients with the Fitbit tracker and brief PA advice. Given that self-monitoring using a simple activity tracker has been consistently demonstrated to be effective in increasing PA levels [45, 49] and that providing PA advice by GPs is considered a standard of care [69, 70], it was deemed unethical to withhold these components from control group participants. Therefore, in the ENERGISED randomised controlled trial [32], Fitbit and brief advice will also be provided to the control group participants. Additionally, this approach enables us to isolate the net effect of the mHealth intervention beyond the activity tracker effect [42].
mHealth interventions typically use smartphone apps or text messages [71]. As (pre)diabetes is associated with older age and lower socioeconomic status [72], a notable segment of (pre)diabetes patients may be unfamiliar with app usage or might not possess a smartphone. Therefore, to ensure the broad accessibility of the intervention, we opted to convey the mHealth component through simple text messages. Text messages have been successfully used in various health interventions [73], including those promoting PA [28, 71]. A recent meta-analysis of mHealth interventions found higher effectiveness of interventions including text messaging, suggesting that it can be explained by their higher intrusiveness when compared with smartphone apps’ notifications [16].
Up until now, most messaging interventions use fixed content that is neither individualised nor adapted to fluctuations in patients’ PA. Furthermore, these messages are typically sent out at pre-defined times that do not respect the ever-changing context of individual patients [28, 71]. Leveraging the latest technological advancements, messages can be delivered just in time and adapted to the immediate context and needs of patients [74]. This precision is achieved by utilising data from sensors, such as those embedded in Fitbit trackers, which offer real-time insights into a patient’s activity patterns [75]. Just-in-time adaptive interventions (JITAIs) have recently been shown as effective in enhancing PA across diverse populations [17, 18, 76]. Examples of just-in-time messages include prompts to increase walking pace triggered when the patient is actively walking or prompts to interrupt sitting when the patient has been sedentary for over 30 min. While the full potential of such intervention can be only realised with a smartphone plus mobile data plan, we’ve ensured inclusivity by accommodating patients with only a basic cell phone with text messaging capabilities. Such patients will receive an adapted version of the mHealth intervention with no just-in-time messages, but equalised in terms of the number and types of messages delivered. This inclusive approach ensures that the intervention is suitable for a diverse range of participants, including older individuals and those from lower socioeconomic backgrounds.
IT solution
To power the mHealth intervention, we have adapted the HealthReact system, developed at the University of Hradec Kralove [32] and compliant with rigorous data governance standards. HealthReact serves as a comprehensive platform to collect, integrate, and evaluate sensor data, particularly from devices like the Fitbit tracker. This seamless integration facilitates the triggering of just-in-time text messages based on real-time Fitbit recorded data. Researchers can select from a broad spectrum of just-in-time triggers that can be tailored to cater to individual patients’ needs. Moreover, the system provides options to set specific parameters governing the delivery of text messages, for instance, regulating the total number of daily messages, defining the minimum interval between two consecutive messages, specifying the time window during which messages are triggered, and setting the likelihood that a triggered message is actually dispatched. This level of granularity ensures that the intervention remains adaptive and patient-centric while also ensuring that participants receive an optimal number of messages.
Phase 2: formative research
Methods
Focus groups were conducted at the premises of two general practices participating in the ENERGISED trial, led by a male PA researcher with PhD and MD degrees (TV) who had no previous relationship with the participants. These focus groups comprised pre(diabetes) patients conveniently sampled from the practices by the respective GP: 7 patients (3 women, age range 53 to 66 years) from the first practice and 7 patients (1 woman, age range 63 to 78 years) from the second. The GPs welcomed the participants, then left and were not present during the focus groups that lasted 55 and 70 min, respectively. As a token of appreciation, participants were given a 20-EUR voucher.
The objective of the focus groups was to refine the key conceptual aspects developed in the previous phase, ensuring the intervention is tailored specifically to the needs and preferences of patients with (pre)diabetes. The topic guide (Additional file 2) included questions about participants’ preferred PA, patterns of sedentary behaviour, and their experiences with using activity trackers and mobile apps.
The focus groups were audio recorded and transcribed verbatim by an independent transcriber. Analysis used thematic analysis with systematic data coding to identify significant patterns and themes. A female qualitative researcher with a PhD degree (KJ) thoroughly read the transcripts, generated initial codes and grouped the codes into potential themes using NVivo software. Themes were reviewed and refined by a second researcher (TV). The analysis was both inductive, driven by the patients’ accounts, and deductive, shaped by conceptual aspects identified in phase 1.
Results
The formative research provided a nuanced understanding of the preferences and challenges faced by individuals with (pre)diabetes regarding PA. These insights informed the customisation of our intervention. Unfortunately, individual participants could not be identified from these focus group transcriptions, so the individual age and gender of those providing quotes cannot be given in this section.
Behaviour change techniques
Goal setting and regular review were supported by the focus group discussions. The participants’ acknowledgement of the motivational impact of setting and achieving PA targets aligns with our intervention’s emphasis on goal setting: “My friend uses a smartwatch to monitor his steps. He’ll notice if he’s only at 8,000 steps and say, ‘I need to reach at least 10,000 steps today,’ and then he’s up and off to achieve it.” This quote illustrates the motivational power of personal goals for behaviour change, a central element of our intervention design.
Feedback on behaviour emerged as a crucial BCT. Participants expressed a preference for feedback that was both affirming and instructive. One participant looked forward to positive reinforcement: “A text message that praises my day’s efforts in the evening and offers encouragement for the next day would be welcome.” Another participant emphasised the importance of reflective feedback to inform future actions: “I’d like an evening summary that evaluates my day, suggesting what I should start or continue doing the next day.” These insights support our intervention’s strategy of providing text messages with tailored feedback to help patients understand their progress and plan subsequent activities.
The concept of social comparison as a BCT elicited mixed reactions. Some participants saw value in a competitive edge: “They have a friendly competition over who was more active, who ran the most, who cycled the most. It certainly motivates.” This suggests that for some, comparing activities with others can be a strong motivator. Conversely, another perspective emphasised self-referenced progress: “I believe that self-comparison is key to personal progress, especially at this age.“, indicating a preference for personal benchmarks over external competition. Given these divergent views, we decided not to include social comparison in our intervention to avoid the potential negative effects of competition and to focus on individual self-improvement, which aligned with our goal of fostering intrinsic motivation.
The focus groups highlighted the importance of understanding the health consequences of PA: “I’m aware that we should all be more active and that I need to lose weight.” This acknowledgement supports the inclusion of educational text messages to inform patients about the health implications of their PA behaviours.
Walking as the primary mode of PA
The focus group discussions provided strong support for walking as the central PA in our intervention. Participants frequently cited walking as a preferred and accessible form of exercise. One participant’s experience highlighted that despite physical health barriers, walking was still seen as a manageable activity to increase: “I do walk and try to maintain a fast pace, but with the weight I’ve gained, even a quick 200-meter walk to the bus leaves me struggling to breathe.” Another participant maintained their walking routine despite unfavourable weather: “My dog ensures we go out for a walk every morning at seven, no matter if it’s raining, snowing, or freezing. We usually walk for half an hour, covering almost the entire block.” This comment not only illustrates the practicality of walking as an exercise that can be integrated into daily life but also shows how external motivation, such as pet ownership, can help overcome environmental barriers like bad weather. These insights collectively affirmed the choice of walking as the primary mode of PA for our intervention.
mHealth and wearables
The formative research phase underscored the potential of mHealth to engage patients with (pre)diabetes in managing their PA. The focus group participants expressed a general openness to using mobile technologies, with many indicating a willingness or interest in using mobile phones or wearables to support their PA goals. One participant articulated a positive stance towards technology: “That would be ideal for me; I’m quite fond of this technology.“, while another highlighted the need for simplicity: “I would be excited to use a pedometer. I’m considering purchasing one, provided it’s not too complex to use.” These insights validate our decision to employ mHealth as a key intervention component, ensuring that it is both accessible and user-friendly.
Just-in-time prompts
The concept of just-in-time prompts was well-received by the focus group participants: “When I’m sitting, and my watch alerts me, it prompts me to stand up, so I do.” This feedback validates our decision to incorporate just-in-time prompts into the intervention, utilising them as immediate nudges towards increased PA and reduced sedentary behaviour.
Phone counselling
The focus group discussions revealed a strong preference for personalised support, which reinforces the inclusion of phone counselling in our intervention. One participant expressed a desire for external motivation: “I would certainly value being more physically active, but it’s something I need to push myself to do, or else have someone else encourage and guide me.” Another participant echoed this sentiment, highlighting the importance of assistance in initiating a healthier lifestyle: “I know I should engage in it, and I would be really grateful for any help I can get to do so.” These statements underscore the value of human interaction in motivating patients to engage in PA and the essential role of counselling in supporting behaviour change.
In summary, the formative research underscored a clear preference for interventions that are not only personalised but also flexible, ensuring they can be adapted to the individual needs and circumstances of those with (pre)diabetes.
Phase 3: pre-testing
Methods
In this phase, we utilised the conceptualisation refined in phase 2 to craft various types of text messages, each incorporating different BCTs. Each type had several specific examples, along with suggestions on how these messages would be triggered. A male PhD student (JN) contacted by phone the seven patients from the second focus group and invited them for face-to-face semi-structured interviews; all invited patients accepted the invitation and participated in the interviews. The interviews were conducted in the researcher’s office and lasted between 25 and 40 min. Participants were given a 20-EUR voucher.
The aim of these interviews was to gather feedback on the sample messages, which would then be used to refine and optimise the messages in alignment with the patients’ preferences and needs. To facilitate this, patients were presented with these sample messages (Table 1), prompting their immediate, think-aloud reactions. The interviews were audio recorded, transcribed verbatim, and subjected to thematic analysis using the same process and involving the same researcher (KJ) as in phase 2. However, unlike in phase 2, only deductive analysis was employed with the themes corresponding to the different types of messages.
Results
Building on the insights from formative research, we developed a series of text messages tailored to leverage specific BCTs (Table 1). The types of messages were as follows:
Walk faster: just-in-time prompts to increase walking pace
Participants responded positively to prompts that encouraged a faster walking pace while they were actually walking. The just-in-time nature of these messages was generally deemed crucial for their effectiveness. One participant expressed enthusiasm for the motivational aspect (Male, 63 years): “Certainly, if it provides motivation, I’d strive to reach the ‘excellent, keep going’ point. That’s the purpose of our walks, to be meaningful.”
Stand up: just-in-time prompts to interrupt sitting
Text messages to interrupt prolonged sitting were seen as potentially very effective. Participants valued the reminder to break their sedentary behaviour, for example, during work hours (Female, 63 years): “I can see myself doing more during work. It would fit well with my routine. But it’s challenging to remember to stand up, so I’d welcome that notification.”
Goal review: an interim review of the patient’s weekly step goal on friday evening
The text message with an interim review of weekly step goals was met with positive feedback, as participants valued the opportunity to reflect on their activity levels. One participant appreciated the self-monitoring aspect, recognising it as a tool for self-improvement (Male, 63 years): “It’s a useful overview. It shows what you’ve accomplished and what’s left to do, giving you a chance to catch up.” This feedback underscores the importance of such notifications in enabling patients to identify when they are falling short of their weekly targets, providing them with the motivation to increase their efforts in the remaining days of the week.
Feedback and encouragement: Sunday evening feedback on the patient’s weekly performance and encouragement for the upcoming week
Most participants valued the text message with feedback on their weekly performance, seeing it as a motivator for the upcoming week (Male, 69 years): “It’s beneficial to have a weekly summary… I can aim to meet or exceed it in the next week,” suggesting that reflective feedback can inspire continued or increased effort. Yet, not everyone was persuaded by the numbers, with one participant stating (Male, 65 years): “My wife might mention, ‘We’ve walked 4,000 steps,’ and I’d respond, ‘That’s irrelevant to me.’ I walk as much as I need, whether it’s 500 steps or 5,000,” indicating a preference for intuitive rather than quantified activity. Despite such views, the consensus leaned towards the usefulness of weekly performance feedback, affirming its inclusion in the intervention.
Action plan reminder: reminders of the action plan adapted to specific plans of each patient
Participants were instructed to suggest their own plans for how and when they wished to incorporate walking into their daily routine (e.g., walking a dog at 7 a.m. or walking home from work at 4 p.m.). The Action Plan Reminder message was then tailored to their individual plans. The desire for tailored messages was evident, with participants suggesting integration with daily routines (Female, 63 years): “If it’s aligned with a regular activity, like brushing teeth in the morning and taking a shower in the evening, then it’s possible to set messages for those times. For instance, I walk my dog every evening at seven; that would be a perfect time for a reminder.” This feedback reinforced the importance of personalising the intervention.
While most message types received positive feedback from participants, the reception of just-in-time messages suggesting an extension of walking distance was mixed. Some participants found them motivating (Female, 63 years): “Absolutely. An extra block would be manageable.” However, others expressed neutral or negative views (Male, 67 years): “I could extend my walk through the village and back. But with heavy shopping, I don’t know,” and (Male, 65 years): “Walking around the house… no, that feels odd.” Consequently, we decided to exclude this type of prompt from the intervention.
Finally, determining the optimal frequency of text messages was crucial to maintaining motivation without causing annoyance. Participants’ preferences varied widely, with some expressing indifference (Male, 65 years): “I don’t know, I don’t care,” while others specified a range (Male, 69 years): “Ideally one or two a day and no more than 10 a week,” and some were open to frequent prompts (Female, 63 years): “Even 6 to 7 a day wouldn’t bother me.” Through this feedback, it became apparent that about 10 notifications per week would be the upper limit to ensure the messages remained a welcome nudge rather than a nuisance.
Phase 4: piloting
Methods
We developed a pilot version of the mHealth intervention and tested it with patients who had prediabetes or uncomplicated type 2 diabetes, were not on insulin therapy, and were regular mobile phone users, meeting the ENERGISED trial eligibility criteria (detailed in Additional file 1). Recruitment was conducted by collaborating GPs as outlined in the ENERGISED trial protocol [32]. In brief, we compiled a list of all patients with (pre)diabetes from participating general practices’ computerised medical records. A random selection of 24 patients was then made from these lists, and GPs introduced the study to all eligible patients opportunistically during routine health check-ups. This process resulted in the recruitment of 10 male patients, 4 with prediabetes and 6 with diabetes, aged between 40 and 76 years. The patients were equipped with the Fitbit Inspire 2 activity tracker [77] and instructed to maintain their typical PA for one week, using the tracker to establish their baseline steps. Subsequently, a researcher contacted them by phone, assisting them in synchronising their tracker with a Fitbit account accessible to the researchers. During this call, a daily step goal was negotiated, and opportunities for integrating walking into their daily routines were discussed, similarly as described in the Final mHealth intervention section. The information collected from this conversation was instrumental in setting up and tailoring the pilot mHealth intervention.
The pilot phase lasted two weeks, during which we monitored the number of text messages patients received. After these two weeks, the same researcher reached out to the patients for brief semi-structured interviews to gather feedback on the intervention’s usability and any potential areas for improvement. Specifically, we asked patients about the frequency, timing, and content of the messages. Patients’ responses and comments were noted during and immediately after the call and were systematically categorised by one of the researchers (TV), who also counted the number of responses per category. Patients participating in the pilot were allowed to keep the Fitbit tracker.
Results
During the pilot, patients received an average of 9.2 ± 10.6 text messages weekly. Five felt the frequency of messages was excessive, and two that they were sometimes sent too closely together. Three patients found the timing of the just-in-time prompts to be ill-suited; for instance, some received prompts to increase their walking cadence after completing their walk. Three participants also expressed inconvenience with receiving prompts to interrupt sitting during work hours when it wasn’t feasible. Lastly, five patients felt that the message content was repetitive.
To address these issues, we implemented several intervention refinements. Specifically, we adjusted the probability of dispatching certain text messages and reduced the maximum number of just-in-time daily prompts (Table 2). This ensures that most patients will receive between three to six messages weekly, with only occasional weeks exceeding ten messages. Additionally, we fine-tuned the parameters for triggering just-in-time prompts related to walking cadence, minimising the likelihood of sending a prompt once walking had finished. However, this adjustment potentially leads to infrequent prompts for patients who engage in minimal walking. To address concerns about receiving prompts to interrupt sitting during work hours, we restricted these prompts to a window between 4 pm and 8 pm. Lastly, to diversify the content and reduce repetitiveness, we crafted multiple text variations for each message type.
Final mHealth intervention
The final intervention comprises six types of text messages, each embodying different BCTs. The individual types, examples of text messages, BCTs utilised, triggering rules, and probability of their dispatch are detailed in Tables 1 and 2. The detailed implementation of the intervention within primary care settings is thoroughly described in the previously published ENERGISED trial protocol [32].
Walk Faster and Stand Up messages are triggered just in time by specific physical behaviour events as detected by Fitbit sensors: 5 min with a step count ranging from 60 to 100 (allowing for one outlier minute below and two above the range) between 8 am and 8 pm for Walk Faster, and 30 min with zero steps while detecting heart rate (to confirm wear) between 4 and 8 pm for Stand Up messages. To prevent overwhelming patients, the frequency of these messages is capped at one per day for Stand Up and two per day for Walk Faster (with a minimum interval of 60 min between them).
Action Plan Reminder messages are triggered according to individual participants’ routines once or more times per week. Goal Review, Feedback and Encouragement, and Health Education messages are triggered at predetermined times once a week, separated throughout the week. Goal Review is triggered on Friday evenings between 8 and 10 pm, allowing participants time over the weekend to catch up. Feedback and Encouragement messages are triggered on Sunday evenings between 6 and 8 pm, offering a review of the past week and motivation for the week ahead. Health Education messages are triggered on Tuesdays between 6 and 8 pm.
Each message’s dispatch is determined by a randomisation algorithm, which decides with a given probability (Table 2) whether the message is actually dispatched to the patient. For instance, the 50% probability of the Goal Review means that the message is triggered every Friday but only dispatched every other week on average. This randomisation not only further limits the weekly text message count but also facilitates the future evaluation of each message’s immediate impact on objectively measured PA levels using a micro-randomised design.
For each message type, there are various text versions from which one is randomly selected (Table 1). Furthermore, the content of Action Plan Reminder messages is tailored to each participant’s individual plans. Goal Review and Feedback and Encouragement messages are also personalised, reflecting each participant’s step count from recent days.
Of note, all standard notifications and prompts typically delivered by the Fitbit wearable and its accompanying app are deliberately deactivated for both intervention and control participants to ensure that they do not interfere with our intervention.
Adapted intervention
For optimal functioning of the intervention, patients require a smartphone compatible with the HealthReact and Fitbit apps (Android 9.0 or iOS 15.0 and later as of November 2023), along with a mobile data plan for continuous internet connectivity. These patients comprise Group A. For participants lacking such resources, the intervention is modified based on the reliability of their Fitbit data syncing:
Group B: Participants in this group who don’t sync their data continuously throughout the day but do sync regularly every day, usually in the afternoon and evening hours (often those without a mobile data plan but with a reliable Wi-Fi connection at home), receive additional time-based Walk Faster messages. This approach compensates for their lack of just-in-time Walk Faster messages due to their syncing patterns.
Group C: Participants who either sync irregularly or not at all (including those with basic cell phones instead of smartphones) are provided additional time-based Walk Faster and Stand Up messages to make up for the absence of just-in-time Walk Faster and Stand Up messages. Furthermore, in these cases, Goal Review and Feedback and Encouragement messages cannot be personalised due to missing recent step count data. Therefore, they receive non-personalised messages that remind them to review their goals and provide encouragement.
Importantly, the adapted intervention is equalised in terms of the number and types of messages delivered. This equalisation is achieved by triggering the adapted time-based Walk Faster and Stand Up messages for Groups B and C only once per day, with the probability of these messages being dispatched set at 15%.
Procedures and counselling
During the baseline visit, all patients (intervention and control) receive a Fitbit Inspire 2 activity tracker from their GP, along with brief PA advice complemented by an educational leaflet and a prescription for PA. Additionally, patients are instructed to maintain their usual PA levels for one more week while wearing the Fitbit to establish their baseline steps.
Approximately one to two weeks later, intervention patients are contacted by phone by a counsellor who assists them in setting individual goals and devising an action plan (e.g., walking a dog for 30 min on three specific days of the week). The counsellor then inputs this information into the HealthReact system to tailor the Action Plan Reminder messages and enable personalisation of the Goal Review and Feedback and Encouragement messages.
In subsequent calls at months 1 to 6 (lead-in phase) to intervention patients, the counsellor supports patients in reviewing their step goals and action plans, employing various BCTs to facilitate goal achievement. During these calls, the counsellor can adjust the mHealth intervention to adapt to the changing needs of the patients. For instance, if patients consistently achieve their step goal, the counsellor may challenge them to increase it. The counsellor also assists patients with technical issues related to the intervention.
From month 7 onwards (maintenance phase), patients no longer receive phone counselling but continue to receive text messages for an additional six months, until month 12, as previously described.
Intervention monitoring
The phone counsellors will review regular weekly reports of their patients’ Fitbit syncing patterns (Fig. 1). Should a patient’s syncing reliability decline, they initially receive a text message from the phone counsellor, prompting regular syncing. If this reminder proves ineffective, the counsellor addresses the issue in the subsequent scheduled call. Persistent syncing challenges may necessitate reassigning the patient to a group with a lower syncing requirement (e.g., from Group A to Group B, or Group B to Group C). Conversely, if patients in Group C or Group B demonstrate improved syncing consistency, surpassing their current group’s requirements, they are upgraded to a more appropriate group (Group B or Group A, respectively). This dynamic approach ensures each participant benefits from the most effective version of the intervention, tailored to their specific mobile phone capabilities and internet access.
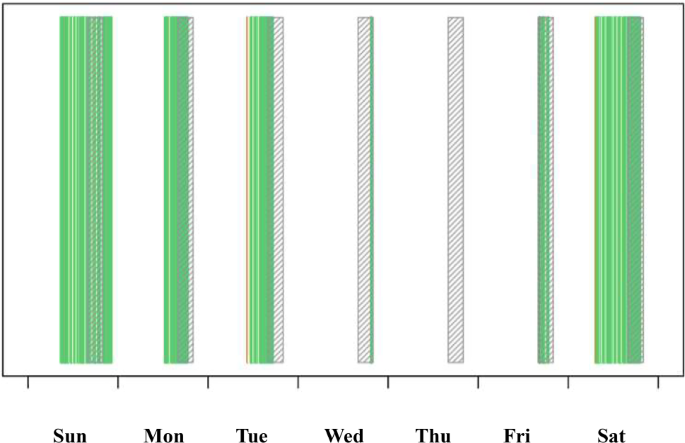
A sample of the weekly report of a patient’s Fitbit syncing pattern. The vertical green lines represent individual Fitbit syncs. The compact green area signifies regular syncing (approx. every 15 min). The hatched area marks time periods from 4 to 8 pm when just-in-time Stand Up text messages are triggered. This specific patient would be classified as Group B: irregular syncing, mostly in the afternoon and during weekends, probably only when connected to the Wi-Fi at home. Despite the irregular sync, the patient would likely receive several just-in-time Stand Up messages per week (assuming she spent 30 min sitting), but hardly any just-in-time Walk Faster messages. Hence, her classification as Group B, which receives adapted Walk Faster messages independent of Fitbit data
link



:max_bytes(150000):strip_icc()/A-Physical-Therapist-Shares-the-Most-Underrated-Physical-Activity-94666d193c98412ca90ffbcc23339f90.jpg)



